Your Guide to TMJ Disorders
What is a TMJ Disorder?
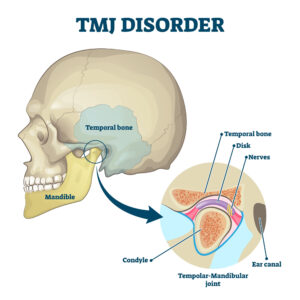
A TMJ disorder indicates an issue in your temporomandibular joints, located on either side of your head near your ears. These joints help your jaw to act as a hinge and work every time you open your mouth to chew, speak, or yawn.
If you hear a popping sound when you open your mouth or feel pain while chewing, this could be a sign of a temporomandibular disorder (TMD). This can make simple actions in your daily life hurt and affect your standard of living.
The Causes of TMD
The TMJ is a complex area of the body, so there are many potential causes of a disorder. Some of the known causes of TMD include:
- The disk slipping out of place
- The disk erodes
- The cartilage around the joint is damaged
- The joint is damaged through impact
At your appointment, Dr. Kaspo will examine your mouth, throat, and jaw to determine if there’s an issue. He’ll ask you about your pain and the issues you’re having to pinpoint an accurate diagnosis.
TMD Symptoms
If you notice the following symptoms, you may have a TMD:
- Pain in your jaw
- Popping or clicking noise when you open your mouth
- Aching pain in or around your ear
- Difficulty chewing
- Pain in your face
- Difficulty opening or closing your mouth
These symptoms and more could be signs that you have an issue with your TMJ.
Treatment for TMD
There are several treatment options available for TMD, and recovery can be improved through multiple treatments used simultaneously. Your treatment may include medication, occlusal therapy, oral orthopedic appliances, physical therapy, or surgery.
Contact Us to Learn More About TMD
If you’re experiencing symptoms that sound like TMD, please contact us by calling (248) 519-1100 or by filling out our online contact form. We’re here for you and we can answer your questions or schedule a consultation for you.
Frequently Asked Questions
What is the main cause of TMJ issues?
The main cause of TMJ issues is a problem with your temporomandibular joints. They’re located on both sides of your head, around the location of your ears. They’re essential for proper jaw movement and when there’s a disorder, everyday actions can hurt.
Your joint can become damaged or weakened in several ways. Some of the most common ways include an injury to the area, due to bruxism (teeth grinding), or arthritis wearing down the cartilage or bone.
How do you fix TMD?
TMD can be fixed through the correction of malocclusion and by strengthening the area around the jaw. You may learn relaxation techniques to avoid putting undue stress on your jaw, as tight muscles can cause TMJ issues.
Rarely, surgery can be used to correct severe jaw issues, but this is reserved as a last case scenario. Most people don’t require surgery to fix their TMD.
Can a TMJ issue go away on its own?
TMJ issues don’t usually go away on their own. It’s best to get an examination of your jaw so you know how severe your TMD is, then follow your dentist’s treatment plan. Trying to treat your TMD on your own can take a long time and your condition may worsen.
Seeing Dr. Kaspo for treatment allows you to start improving your TMD sooner and reduces your risk of serious issues. He’ll develop an effective treatment plan for you that addresses your pain and other problems you’re having with your jaw.